Can You Get Dry Socket With Sutures

Hey there, lovely people! So, you’ve recently had a dental procedure – maybe a wisdom tooth extraction, a root canal, or something that left your mouth feeling a little…stitched up. You’re probably navigating the post-op world with a newfound appreciation for soft foods and a cautious approach to anything remotely crunchy. And then, like a pop-up ad you didn't ask for, the phrase “dry socket” pops into your mind. It’s a bit of a dental boogeyman, isn't it? But here’s the burning question many of you might be quietly pondering: can you actually get dry socket if you have sutures in place? Let’s dive in, shall we?
Think of your mouth as a bustling city. After a dental procedure, especially one requiring sutures, it’s like there’s been some major construction. The stitches are like temporary barriers, holding things together while the real repair work – the healing – gets underway. They’re designed to keep everything neat and tidy, guiding the tissue to knit back together smoothly. So, does the presence of these helpful little stitches completely shield you from the dreaded dry socket?
Let’s get straight to the point. The short answer is: yes, you absolutely can still get dry socket, even with sutures.
Must Read
Now, before you start picturing a dire scenario worthy of a medical drama, let’s unpack this a little. Dry socket, or alveolar osteitis, is a rather unpleasant complication that can occur after a tooth extraction. Normally, after an extraction, a blood clot forms in the empty tooth socket. This clot is your mouth’s natural superhero, acting as a protective shield for the underlying bone and nerves. It’s the starting point for healing. Dry socket happens when this crucial blood clot either doesn’t form at all, or it gets dislodged or dissolves prematurely.
Imagine that blood clot as a little thatched roof over a sensitive area. If that roof is blown away or never built, the exposed “house” (your bone and nerves) is left vulnerable to the elements – in this case, air, food particles, and bacteria. This can lead to intense pain, often radiating to the ear, and a generally yucky feeling. It’s definitely not the chill vibe we’re aiming for during recovery.
So, how do sutures fit into this picture? Well, sutures are fantastic for holding the gum flaps together, especially after complex extractions or when multiple teeth are removed. They help to stabilize the area, reduce gaping, and can sometimes make the initial healing feel a bit more contained. For many, they offer a sense of security. They’re like the cheerful scaffolding on a building under renovation.

However, those stitches, as helpful as they are, don't magically prevent the blood clot from forming or staying put. The core issue with dry socket is the integrity of that initial blood clot. If the conditions are right – and by “right” we mean “wrong” for healing – that clot can still be compromised, regardless of whether your gums are neatly stitched.
What are these “conditions” that can lead to a compromised clot? It’s often a combination of things. Aggressive spitting or rinsing in the first 24-48 hours is a big no-no. Think of it like trying to dry your freshly washed hair by violently shaking it – not ideal for delicate processes. Likewise, smoking or using straws creates suction that can literally suck that precious blood clot right out of its socket. It’s like using a vacuum cleaner on your tender healing wound. Ouch.
Certain medications, like oral contraceptives, can also influence clot formation and stability. And then there’s the classic culprit: poor oral hygiene. If food debris or bacteria get into the socket area, they can irritate and potentially break down the clot. This is where those sutures can sometimes be a double-edged sword. While they help keep things closed, they can also trap food particles if you’re not careful. It’s a bit like a poorly managed backpack; things can get stuck in the nooks and crannies.
So, even with sutures holding your gums in place, if you engage in any of these clot-disrupting activities, the underlying socket can still become exposed and develop dry socket. The sutures are a bandage for the gum tissue, but the dry socket is about what’s happening deeper down in the socket itself.

Your dentist or oral surgeon will give you specific post-operative instructions. Following these instructions to the letter is your superpower against dry socket. This usually involves a gentle approach. For rinsing, they’ll likely advise you to avoid vigorous spitting. Warm salt water rinses are often recommended, but typically after the first 24 hours, and they should be done with extreme gentleness. Imagine pouring delicate tea, not power washing your driveway.
And speaking of gentle, let’s talk about what you’re eating. Think of your mouth as a five-star spa during this recovery period. Soft, non-irritating foods are your best friends. We’re talking smoothies (no straws!), yogurt, mashed potatoes, soups (lukewarm, not hot!), and scrambled eggs. Avoid anything small, hard, or crunchy that could lodge itself in the socket or under your stitches. No popcorn kernels, no tiny seeds, and definitely no super-chewy caramels. Your future, pain-free self will thank you.
The role of sutures in preventing dry socket is more about indirect protection. By keeping the gum edges together, they can help reduce the likelihood of food particles or bacteria directly entering the socket. They create a more sealed environment, which is generally conducive to healing. Think of it like a well-maintained fence around a garden. It keeps out the wandering animals and helps the plants grow undisturbed. But, if a storm comes (like aggressive rinsing or smoking), the fence might hold, but the delicate flowers inside can still be damaged.
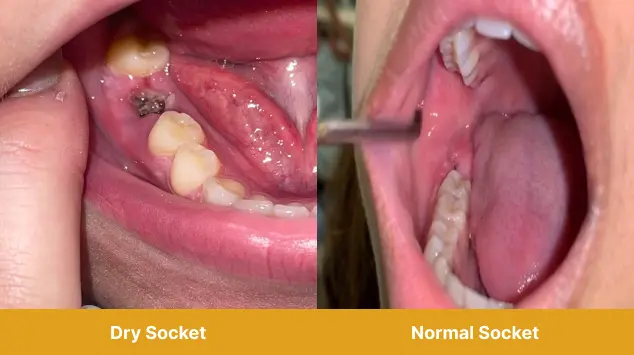
Here’s a fun fact for you: the term “dry socket” itself is quite literal. It describes the dry, exposed bone that becomes visible and painful when the protective blood clot is gone. It's a bit like finding a perfectly formed, empty bird's nest after a strong wind – fascinating in its own way, but not where you want it to be in your mouth.
Cultural references? Think about how different cultures approach healing. In many traditional practices, there’s a deep respect for the body’s natural healing processes, often involving rest, gentle care, and specific remedies. While dry socket is a modern dental issue, the principles of gentle care and avoiding irritation are timeless. It’s like the ancient wisdom of “listen to your body” applied to a contemporary dental situation.
So, what does this mean for you, navigating the suture-filled landscape of your post-dental recovery? It means staying vigilant, even with the comfort of those stitches. Your dentist is your guide, and their instructions are your roadmap. Don’t be shy about reaching out if you have concerns. A little extra reassurance or a quick check-in can save you a world of discomfort.
If you start experiencing severe, throbbing pain that doesn’t subside with over-the-counter pain relievers, or if you notice a foul taste or smell, contact your dentist immediately. They can diagnose dry socket and treat it effectively. Treatment often involves a gentle irrigation of the socket and the placement of a medicated dressing, which can bring immediate relief. It’s like giving that exposed bone a soothing balm.
Remember that sutures themselves are usually made of dissolvable material, or they’ll be removed by your dentist at a follow-up appointment. As they do their job and eventually disappear or are removed, the healing tissue beneath will (hopefully!) have done its job too, having formed its own protective layer.
It’s a delicate dance, this healing process. The sutures are a significant part of the support system, helping to keep the gum tissue in its optimal position. They are excellent at preventing flap displacement and promoting early tissue approximation. However, they are not a foolproof shield against the specific mechanisms that cause dry socket. It's a bit like wearing a stylish, well-fitted jacket. It looks great and offers a layer of protection, but it doesn’t mean you can’t still get a chill if you stand outside in a blizzard without adequate preparation.
The emphasis, always, is on protecting that blood clot. Everything you do – or don’t do – in the days following your procedure contributes to its formation and stability. Gentle handling, avoiding irritants, and proper oral care are the cornerstones of a smooth recovery, sutures or no sutures.
Ultimately, life is full of these little reminders to be mindful and gentle with ourselves. Whether it’s recovering from dental work, navigating a tricky relationship, or simply trying to get through a busy week without spontaneously combusting, the principle of gentle care often serves us best. Those sutures are a physical manifestation of that care, reminding us that our bodies are capable of incredible repair, but they appreciate a little help and a lot of kindness along the way. So, sip that smoothie, take a gentle rinse, and trust the process – your mouth will thank you for it, stitches and all.


